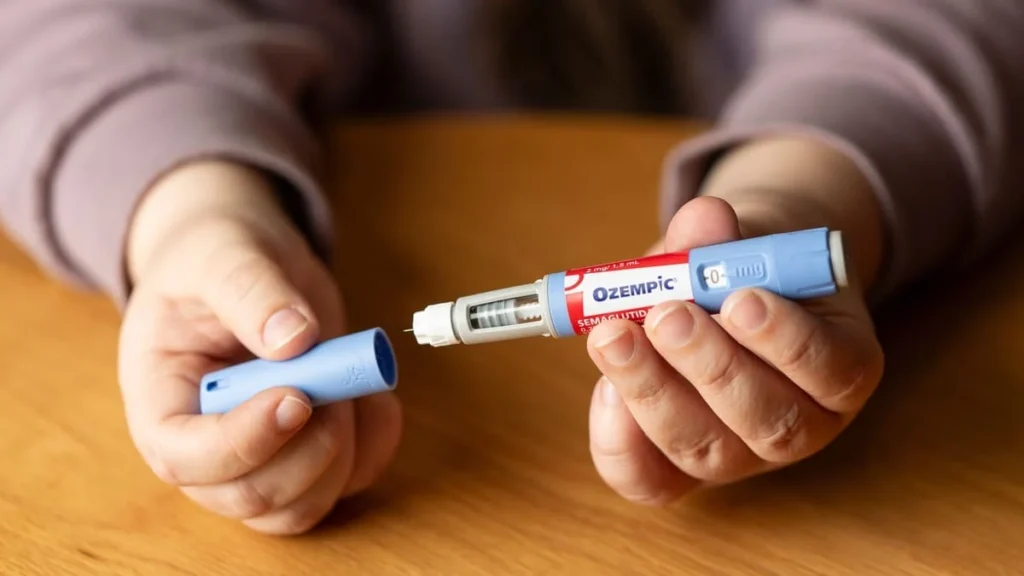
PricewaterhouseCoopers (PwC) in the United States has announced a significant change to its employee benefits program, citing "rapidly rising costs" as the primary driver for discontinuing coverage of popular weight loss medications. Effective from July, only employees diagnosed with type 2 diabetes will be eligible for glucagon-like peptide-1 (GLP-1) medicines, such as Ozempic and Mounjaro, which have seen an explosion in demand for their efficacy in weight management. This move by one of the Big Four accounting firms highlights a growing tension between employers’ desire to offer comprehensive health benefits and the unsustainable financial burden posed by increasingly expensive pharmaceutical treatments.
Employees discovered the impending changes during their annual benefits renewal process, leading to immediate concern and frustration among those who rely on these medications for weight management. One PwC employee, speaking to the Financial Times, which first reported the decision, voiced a sentiment echoed by many: "We work so hard and do such long hours sitting in front of a computer, it is not conducive to an active lifestyle. I don’t think the obesity diagnosis is being treated respectfully." This reaction underscores a deeper debate about the nature of obesity as a chronic disease and the role of corporate responsibility in supporting employee health beyond basic medical necessities.
The Phenomenon of GLP-1 Agonists: A Medical Breakthrough and Financial Challenge
The medications at the heart of this controversy, GLP-1 receptor agonists, were initially developed and approved for the treatment of type 2 diabetes. Drugs like Ozempic (semaglutide) and Mounjaro (tirzepatide) effectively help control blood sugar levels by mimicking a natural hormone that regulates insulin secretion and slows gastric emptying. However, a significant side effect observed in clinical trials was substantial weight loss, leading pharmaceutical companies to seek and obtain additional approvals for dedicated weight management formulations, such as Wegovy (semaglutide for weight loss) and Zepbound (tirzepatide for weight loss).
These drugs have been hailed as a revolutionary advancement in the fight against obesity, a chronic condition affecting more than 42% of adults in the United States, according to the Centers for Disease Control and Prevention (CDC). Clinical studies have demonstrated that patients can achieve an average weight reduction of 15-20% of their body weight, significantly improving obesity-related comorbidities like hypertension, dyslipidemia, and obstructive sleep apnea. This unprecedented efficacy, coupled with extensive media coverage and celebrity endorsements, has propelled GLP-1s into the public consciousness, creating immense demand.
However, the medical marvel comes with a hefty price tag. Without insurance, a month’s supply of these medications can cost anywhere from $900 to $1,300 in the US. While the UK market might see slightly lower figures, around £300 a month for stronger doses, the cumulative cost across a large workforce can quickly escalate into millions of dollars annually for a self-insured employer. Given that obesity affects a substantial portion of the adult population, the potential pool of eligible employees for weight loss drugs is vast, far exceeding the number of individuals with type 2 diabetes.
A Chronology of Rising Costs and Employer Responses
The trajectory of GLP-1 coverage in employer-sponsored health plans has been swift and dramatic. When these drugs first gained traction for weight loss around 2021-2022, many progressive employers, recognizing the potential long-term health benefits and associated reduction in future healthcare costs for chronic diseases linked to obesity, began including them in their pharmacy benefits. The hope was that proactive weight management could lead to a healthier workforce, reduced absenteeism, and improved productivity.
By late 2022 and early 2023, however, the financial implications began to crystallize. Research, such as that conducted by Blue Cross Blue Shield, a major US not-for-profit health insurer, revealed the staggering impact. Their analysis last year indicated that including GLP-1 medications in coverage could increase employers’ insurance premiums by as much as 14%. This significant jump, far exceeding typical annual increases in healthcare costs, forced a re-evaluation of benefit strategies.

PwC’s decision, therefore, is not an isolated incident but rather a reflection of a broader industry trend. Earlier this year, Blue Cross Blue Shield itself announced that it would cease covering weight-loss drugs for its own employees unless they had a diabetes diagnosis, explicitly stating that spiraling costs had become an "unsustainable burden." This move by a major insurer to restrict coverage for its own staff signaled a coming wave of similar decisions across the corporate landscape. Other companies, both large and small, are reportedly scrutinizing their benefit plans, weighing the substantial costs against employee well-being and fiscal responsibility. The average annual increase in employer-sponsored health insurance premiums for 2023 was around 7%, but the impact of GLP-1s pushed this much higher for those offering comprehensive coverage.
Official Stances and the Nuance of Clinical Necessity
PwC US, in its official statement, confirmed its revised policy, emphasizing that it would continue to cover GLP-1 medication "when prescribed for conditions aligned with established standards of care, such as type 2 diabetes." Crucially, the firm clarified that these drugs "will not be included under pharmacy coverage for weight management." This distinction is pivotal, as it frames the decision not as a denial of essential medication but as a re-alignment with established clinical guidelines for specific diseases.
The firm further explained that the change "reflected broader industry trends and the need to manage rapidly rising costs, while maintaining access to clinically necessary treatments." It committed to monitoring the "external landscape to make thoughtful benefits decisions that will support our people broadly and help keep coverage sustainable over time." This language suggests a cautious approach, acknowledging the sensitivity of the issue while prioritizing long-term financial viability of their benefits program.
The situation contrasts with the UK, where healthcare systems differ significantly. A spokeswoman for PwC UK confirmed that employees in the UK typically do not have access to weight-loss drugs through its private medical insurance. This is largely consistent across the "Big Four" accounting firms in the UK, where private medical insurance often supplements the National Health Service (NHS) rather than being the primary provider of comprehensive care for all conditions. The NHS itself has limited access to GLP-1s for weight management, typically reserved for severe obesity with specific co-morbidities and managed through specialized weight management services.
Employee Morale and Ethical Dilemmas
The impact on employee morale and the ethical implications of such benefit cuts are profound. For employees who have started GLP-1 treatments and experienced significant health improvements, the sudden withdrawal of coverage can be devastating, forcing them to either pay thousands out-of-pocket or discontinue treatment, potentially leading to weight regain and a return of health issues. The employee’s quote about the disrespect shown to an "obesity diagnosis" highlights a critical tension: while medical science increasingly recognizes obesity as a chronic disease requiring ongoing treatment, benefit policies often struggle to keep pace with this understanding, especially when costs are high.
Human resources departments face a significant challenge in balancing cost containment with employee well-being and maintaining a competitive benefits package. In an era where companies are vying for top talent, attractive benefits are a key differentiator. Decisions like PwC’s, while financially prudent, risk alienating employees and potentially impacting talent retention, especially for a firm that expects long hours from its staff. HR experts suggest that such decisions must be communicated with extreme sensitivity, clarity, and an emphasis on alternative support mechanisms, even if direct drug coverage is withdrawn. The conversation also extends to preventative care – if employers are unwilling to cover expensive treatments, what investments are they making in promoting active lifestyles and healthy eating within the workplace to prevent obesity in the first place?
Broader Implications and Future Outlook
PwC’s decision is a bellwether for the future of employer-sponsored health benefits in the US. The implications are far-reaching:
- For Employees: Many will face difficult choices. Those who can afford the out-of-pocket costs may continue treatment, exacerbating health disparities. Others may have to cease medication, potentially experiencing weight regain and a decline in health, leading to increased long-term healthcare utilization for obesity-related conditions. This could foster resentment and a feeling of being undervalued by their employer.
- For Employers: While short-term cost savings are a clear motivation, the long-term impact on workforce health, productivity, and morale remains to be seen. Companies might find themselves in a challenging position, balancing the financial bottom line with their commitment to employee welfare and their public image as responsible corporate citizens. The competitive landscape for talent might force some to reconsider or offer alternative, less costly, weight management programs.
- For the Healthcare System: The debate over GLP-1 coverage highlights the systemic issues within the US healthcare system, particularly the tension between pharmaceutical innovation and affordability. It places pressure on drug manufacturers to potentially lower prices or face reduced market access through employer plans. It also reignites discussions about the role of insurance companies and Pharmacy Benefit Managers (PBMs) in negotiating drug costs and managing formularies.
- For Public Health: The widespread adoption of GLP-1s had offered a glimmer of hope in addressing the obesity epidemic. Restricting access through employer benefits could slow progress, widening the gap between those who can afford effective treatment and those who cannot. This raises questions about public health policy and whether these "miracle drugs" should be considered essential, potentially leading to calls for government intervention or subsidies.
The unfolding situation with GLP-1 coverage marks a critical juncture in corporate benefits strategy. As pharmaceutical science continues to deliver innovative, yet expensive, treatments for chronic conditions, employers will increasingly grapple with how to balance financial sustainability with a genuine commitment to employee health. PwC’s move, while pragmatic from a cost-management perspective, ignites a broader conversation about the definition of "clinically necessary," the responsibilities of employers, and the evolving landscape of healthcare in the 21st century. The external landscape, as PwC noted, will indeed be closely monitored by all stakeholders as this complex issue continues to develop.