Employer-sponsored health insurance costs are projected to experience their highest increase in 15 years, with a significant 6.7% rise anticipated for 2026. This surge is expected to push the average annual expense per employee beyond $18,500, marking a critical juncture for businesses grappling with escalating healthcare expenditures. The projections, derived from Mercer’s 2025 National Survey of Employer Sponsored Health Plans, highlight a mounting financial burden that is increasingly impacting corporate bottom lines and broader business operations. Mercer, a subsidiary of Marsh McLennan and a leading advisor on workforce issues, emphasized that this 6.7% figure represents the expected average increase after employers implement planned cost-saving measures. Without such interventions, the anticipated average increase would have been over 9%, a rate that would outpace the Consumer Price Index by five to six percentage points.
A Decade of Growth Accelerates: The Financial Strain on Employers
The current elevated cost trend is not an isolated incident but rather an acceleration of a pattern that began in 2023. This follows a decade where annual growth in health insurance costs averaged a comparatively modest 3%. The shift from gradual increases to a rapid acceleration poses a significant challenge for organizations, pressuring benefit budgets and, in some cases, beginning to influence wider business strategies. The report underscores that while general inflation for other goods and services has shown signs of cooling, the healthcare trend is moving in the opposite direction, creating a "red flag for CFOs," as noted by Beth Umland, director of health research at Mercer US.
The growing unease among finance leaders is palpable. The share of CFOs identifying healthcare as a top three concern has surged from 19% in 2024 to a striking 33% for 2026. This nearly doubling of concern within a two-year span reflects the intensifying pressure. Umland further explained via email that "In addition, health care claims cost has been increasingly volatile, making it harder for organizations with self-funded plans to manage their budgets." This volatility, coupled with accelerating costs, introduces an element of unpredictability that complicates financial planning and risk management for companies, particularly those that bear the direct financial risk of their employees’ healthcare claims.
Employer Strategies for Cost Mitigation and Plan Redesign
In response to these daunting projections, employers are actively seeking strategies to curb rising costs without entirely eroding employee benefits. The Mercer survey, which polled 161 CFOs and other finance professionals in February, revealed a strong inclination towards modifying plan designs. Nearly half of the surveyed finance leaders indicated a preference for changes such as higher deductibles or restructured cost-sharing mechanisms. These adjustments aim to shift a greater portion of the immediate cost burden to employees at the point of service, thereby potentially reducing overall plan expenditures.
However, there’s a notable reluctance among CFOs to increase employee premium contributions. This hesitancy likely stems from a desire to maintain competitive benefits packages and avoid negatively impacting employee morale or financial well-being. Raising premiums directly affects every employee enrolled in the plan, often leading to greater dissatisfaction than changes in deductibles or co-pays, which might only affect those who utilize healthcare services frequently. This delicate balance highlights the complex decision-making process employers face: how to manage escalating costs while simultaneously attracting and retaining talent in a competitive labor market.
The GLP-1 Factor: A Double-Edged Sword in Healthcare Spending
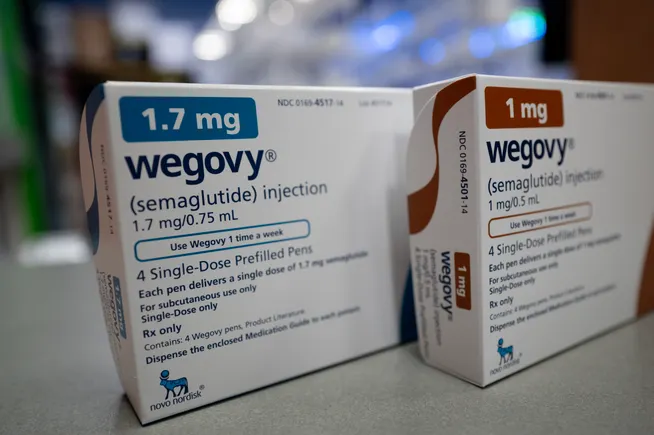
One of the most significant and rapidly evolving factors contributing to healthcare spending trends is the advent and widespread adoption of GLP-1 (Glucagon-Like Peptide-1) drugs. These medications, primarily used for conditions such as Type 2 diabetes and increasingly for weight management, come with a substantial price tag, typically ranging between $1,000 and $1,500 per month for consumers. Employers often bear a significant portion of this cost, covering 70% to 100% of the expense, according to a January SHRM article.
The impact of GLP-1 drugs on national healthcare expenditure is already evident. Data from the Kaiser Family Foundation analysis of claims reveals that Medicare spending on GLP-1 drugs surged to approximately $27.5 billion in 2024, a staggering increase of more than five times the spending recorded in 2019. This exponential growth in spending within the Medicare system serves as a powerful indicator of the broader financial implications these drugs are having across all healthcare payers, including employer-sponsored plans.
Currently, about half of large employers (those with 500 or more employees) offer coverage for GLP-1s specifically for weight management. This trend of increasing coverage has been observed over the past three years. However, Mercer anticipates a potential slowdown or even a halt in this expansion for 2026 as employers intensify efforts to control high cost increases. Umland elaborated on this, stating, "Those that currently provide this coverage are evaluating all methods for managing utilization, from eligibility controls that help ensure the medications are used by those who will benefit most, to requiring participation in a support program that will help ensure members who do use these medications are positioned to get the maximum benefits." These utilization management strategies reflect a proactive approach by employers to ensure that expensive treatments are both medically appropriate and deliver the intended health outcomes, thereby maximizing the return on their benefits investment.
Historical Context and Macroeconomic Pressures on Healthcare Costs
The current situation is not merely a short-term blip but the culmination of various historical trends and contemporary economic forces. For over a decade leading up to 2023, employer-sponsored health insurance costs saw relatively stable, albeit consistent, annual increases averaging around 3%. This period was characterized by incremental adjustments and a focus on managing chronic conditions more efficiently. However, the post-pandemic economic landscape has introduced new variables that have fundamentally altered this trajectory.
The acceleration in healthcare costs observed since 2023 can be attributed to several interconnected factors. First, broader economic inflation, while cooling in some sectors, has persistently affected the healthcare industry. Labor shortages, particularly among nurses and other skilled medical professionals, have driven up wages, which in turn are passed on through higher service costs. Supply chain disruptions, though easing, have also contributed to increased costs for medical supplies, equipment, and pharmaceuticals.
Furthermore, advancements in medical technology and new drug therapies, while offering improved patient outcomes, often come with premium price tags. The emergence of highly effective but expensive medications like GLP-1s exemplifies this dynamic. These innovations represent a double-edged sword: they enhance patient care and quality of life but simultaneously place immense pressure on healthcare budgets. The aging workforce and a rise in chronic disease prevalence also contribute to higher utilization of healthcare services, further exacerbating the cost challenge.
Implications for Businesses, Employees, and the Broader Economy
The projected surge in health insurance costs carries profound implications for various stakeholders. For businesses, higher benefits expenses directly impact profitability and can influence strategic decisions regarding investment, expansion, and even workforce size. Companies operating on tighter margins may find themselves in a difficult position, forced to make tough choices between absorbing increased costs, passing them on to employees, or re-evaluating their benefits offerings. This also affects their competitiveness in the market, both in terms of product pricing and talent attraction. A company unable to offer competitive health benefits may struggle to recruit and retain skilled employees, particularly in sectors where benefits are a major differentiator.
For employees, the implications are equally significant. While employers may be reluctant to increase premium contributions, the shift towards higher deductibles and modified cost-sharing structures means that employees will likely bear a greater share of out-of-pocket expenses. This can have a direct impact on household budgets, potentially leading to delayed care, medical debt, or financial strain, especially for those with chronic conditions or unexpected health crises. The affordability of healthcare becomes a critical concern, influencing employees’ financial well-being and overall job satisfaction. The delicate balance for HR departments lies in navigating these cost pressures while simultaneously ensuring that benefits remain valuable and accessible to employees.
On a broader economic scale, escalating healthcare costs contribute to national healthcare expenditure, which in the U.S. already accounts for a significant portion of the GDP. This can have ripple effects on consumer spending, inflation, and the overall economic health of the nation. The trend underscores the ongoing need for systemic reforms and innovative solutions to address the fundamental drivers of healthcare costs.
Beyond the Numbers: Future Outlook and Potential Solutions
In anticipation of these challenges, many employers are looking beyond traditional plan design changes to more innovative strategies. These include:
- Wellness Programs: Investing in comprehensive wellness programs designed to promote preventive care, healthy lifestyles, and chronic disease management can potentially reduce future healthcare utilization and costs.
- Telehealth Expansion: Continued expansion and promotion of telehealth services can offer more convenient and often more cost-effective access to care for certain conditions, reducing reliance on expensive emergency room visits or specialist consultations.
- Direct Contracting and Centers of Excellence: Some larger employers are exploring direct contracts with healthcare providers or establishing "centers of excellence" for specific high-cost procedures (e.g., organ transplants, orthopedic surgeries). These arrangements aim to negotiate better rates and ensure high-quality care, thereby improving outcomes and reducing overall costs.
- Price Transparency Tools: Empowering employees with tools to compare prices for services and procedures can encourage more cost-conscious healthcare decisions.
- Data Analytics: Utilizing sophisticated data analytics to identify cost drivers, predict future trends, and tailor interventions can help employers make more informed decisions about their benefits strategies.
The projected 6.7% increase in employer-sponsored health insurance costs for 2026 serves as a stark reminder of the persistent and accelerating challenges in the U.S. healthcare system. It necessitates a multi-faceted approach from employers, involving strategic plan design, vigilant management of emerging cost drivers like GLP-1 drugs, and a commitment to exploring innovative solutions. The Mercer survey’s findings underscore that navigating this complex landscape will require adaptability, careful financial planning, and a continued focus on balancing cost control with the imperative of providing valuable healthcare benefits to employees.