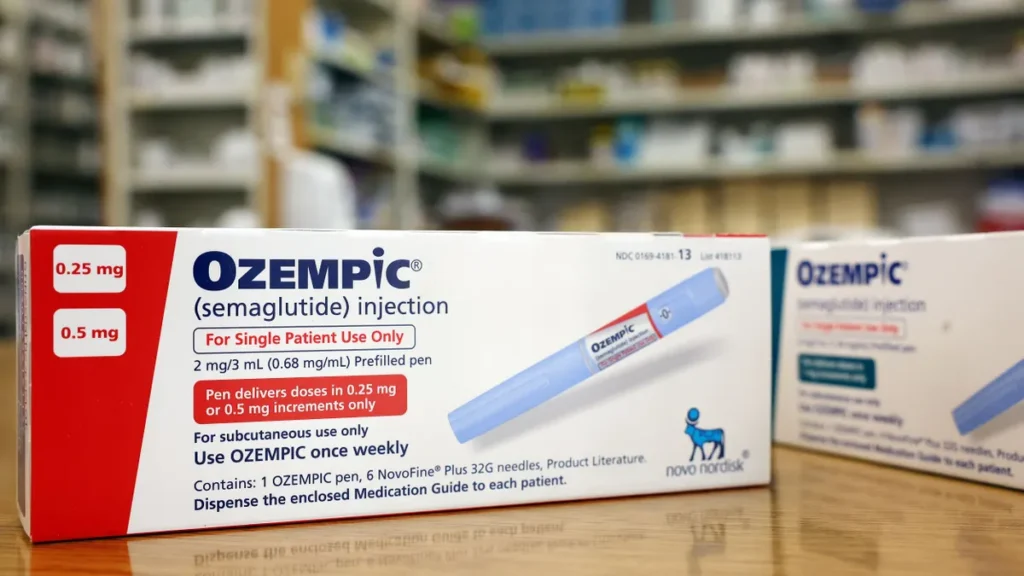
The financial viability of glucagon-like peptide-1 (GLP-1) medications, widely used for diabetes and increasingly for weight management, is a source of "tremendous concern" for companies across the United States. This sentiment, articulated by Ellen Kelsay, president and CEO of the Business Group on Health, underscores a looming crisis in corporate healthcare budgets, which are already bracing for anticipated double-digit increases in overall healthcare costs. The rapid adoption and high price point of GLP-1s like Ozempic, Wegovy, Mounjaro, and Zepbound are profoundly reshaping how employers approach their health benefits strategies, forcing a difficult balancing act between employee well-being and fiscal responsibility.
The Transformative Rise of GLP-1 Medications
GLP-1 receptor agonists represent a groundbreaking class of pharmaceuticals that have revolutionized the treatment of Type 2 diabetes and chronic weight management. Originally developed for diabetes, these drugs mimic the action of a natural hormone, GLP-1, to stimulate insulin release, suppress glucagon secretion, slow gastric emptying, and promote satiety. This multifaceted action leads to improved blood sugar control and significant weight loss, offering hope to millions struggling with these pervasive health conditions.
The journey of GLP-1s began with drugs like exenatide (Byetta, approved 2005) and liraglutide (Victoza, approved 2010), primarily for Type 2 diabetes. However, it was the subsequent approvals for weight management that catapulted them into the public consciousness and onto employer benefits radars. Liraglutide was approved as Saxenda for chronic weight management in 2014. More recently, semaglutide, initially approved as Ozempic for diabetes in 2017, received FDA approval as Wegovy for weight management in 2021. This was followed by tirzepatide, approved as Mounjaro for diabetes in 2022 and later as Zepbound for weight management in 2023. These newer generations of GLP-1s have demonstrated even more potent effects on weight loss, further amplifying their demand and, consequently, their impact on healthcare spending.
The effectiveness of these medications is undeniable. Clinical trials have shown significant average weight loss—upwards of 15% for Wegovy and even higher for Zepbound—alongside improvements in cardiovascular risk factors and overall metabolic health. This efficacy has driven unprecedented demand, with prescriptions surging across demographic groups. However, this medical breakthrough comes with a substantial price tag. Monthly costs for these medications can range from $900 to over $1,300, translating to annual expenses of $10,000 to $16,000 per patient. When scaled across a large employee population, even a modest uptake can lead to astronomical increases in a company’s healthcare expenditure.
Mounting Financial Pressures and the Affordability Crunch
The core of the employer dilemma, as highlighted by Ellen Kelsay, lies in the "significant implications for health care budgets and overall affordability" stemming from GLP-1s and the broader rise in prescription drug costs. Historically, annual increases in employer-sponsored health benefits have hovered in the mid-single digits. However, recent projections, including those from Mercer in November, have warned of a "healthcare affordability crunch" with anticipated double-digit increases. This surge is fueled in large part by the escalating costs of GLP-1 medications, which represent a new frontier of high-cost, high-demand treatments.
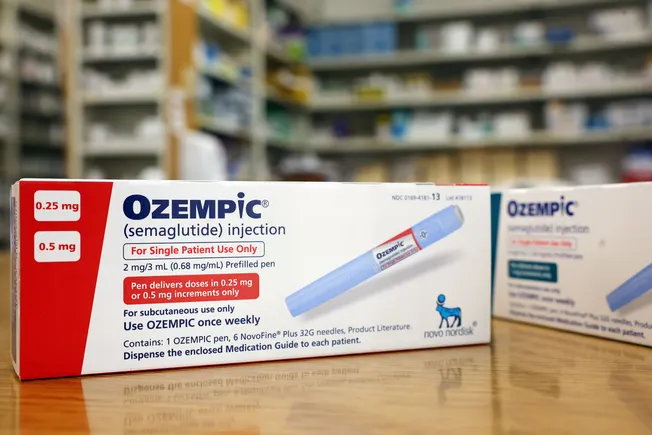
For many companies, healthcare benefits are one of the largest expenses after salaries. A sudden, substantial increase in these costs directly impacts profitability, resource allocation, and even the ability to offer competitive compensation packages. Human resources and finance departments are therefore under immense pressure to find sustainable solutions without compromising employee health or company culture. The Business Group on Health’s survey, conducted in February and March among 105 employer members, provided concrete evidence of this widespread concern, indicating that the issue is not theoretical but an immediate and pressing challenge.
The economic implications extend beyond direct drug costs. Increased utilization of GLP-1s can also lead to higher administrative fees for pharmacy benefit managers (PBMs) and increased demand for associated medical services, such as specialist consultations (endocrinologists, bariatric specialists) and diagnostic tests. While some argue that these upfront costs could be offset by long-term savings from reduced incidence of obesity-related comorbidities like Type 2 diabetes, heart disease, stroke, and certain cancers, these savings are speculative and occur over a much longer horizon, offering little immediate relief to strained annual budgets.
Strategies for Cost Containment: The "Guardrails" Implemented by Employers
In response to these escalating costs, many companies are implementing stringent "guardrails" to manage the use and expenditure on GLP-1 medications. These strategies aim to ensure "appropriate use" by targeting individuals who stand to benefit most clinically, while simultaneously controlling the financial outflow. The Business Group on Health survey identified several common approaches:
-
Clinical Eligibility Using Objective Biometric Data: Employers are increasingly requiring robust medical documentation to justify GLP-1 prescriptions. This often includes specific Body Mass Index (BMI) thresholds (e.g., BMI ≥30, or BMI ≥27 with at least one weight-related comorbidity like hypertension or dyslipidemia), along with a history of failed attempts at physician-supervised weight loss. This criterion aims to align coverage with FDA-approved indications and medical necessity guidelines, preventing purely cosmetic use.
-
Mandatory Participation in a Weight Management Program: To promote a holistic approach to health and ensure sustained lifestyle changes, many companies are mandating that employees enrolled in GLP-1 coverage also participate in structured weight management programs. These programs typically involve nutritional counseling, physical activity guidance, behavioral therapy, and regular check-ins with healthcare professionals. The rationale is that medication should be a tool within a broader framework of lifestyle modification, not a standalone solution. This also helps ensure that employees are educated about potential side effects and the importance of adherence.
-
Limiting Prescribing to Certain Providers: Some employers are restricting GLP-1 prescriptions to specialists such as endocrinologists or bariatric physicians, or those with specific certifications in obesity medicine. This measure aims to ensure that complex weight management cases are handled by experts who can provide comprehensive care, monitor for contraindications, and manage potential side effects, rather than by general practitioners who may have less specialized experience in this rapidly evolving field. This also helps to curb indiscriminate prescribing.
-
Excluding Certain Medications from the Formulary: While less common for the most impactful GLP-1s, some companies may choose to exclude specific brand-name GLP-1s or restrict coverage to only those indicated for diabetes, not weight management, if a particular drug has dual indications. This highly controversial strategy, however, can lead to significant employee dissatisfaction and potential health inequities. More often, exclusions might target newer, even higher-priced GLP-1s until their long-term efficacy and cost-effectiveness are better established.

Despite the implementation of these comprehensive guardrails, the survey revealed that even these measures "don’t do enough to ease cost pressures" on some companies’ healthcare budgets. This indicates the sheer magnitude of the financial challenge and suggests that current mitigation strategies may only be partially effective or that the underlying demand and cost structure of GLP-1s are simply too high for conventional controls to fully contain.
The Employee Experience: Access, Affordability, and Adherence Challenges
The financial strain on employers inevitably trickles down to employees, profoundly impacting their access to these life-changing medications. The Employee Benefit Research Institute (EBRI) released a survey in March, revealing that more than a third of GLP-1 users had stopped taking their medication. A significant 40% cited cost as the primary reason for discontinuation, while approximately 1 in 7 pointed to a complete lack of coverage for the medication.
This data paints a stark picture of the challenges faced by individuals. Even with employer coverage, high deductibles, co-pays, and co-insurance can make long-term adherence financially untenable for many. The requirement for continuous use for sustained benefits means that any interruption due to cost can negate previous progress and lead to weight regain or worsening diabetes control. This creates a deeply personal and often frustrating dilemma for employees who have found effective treatment but cannot sustain it financially.
The lack of consistent coverage also raises significant health equity concerns. Access to these effective treatments can become a privilege rather than a right, potentially exacerbating existing health disparities based on income, employment status, and insurance plans. Employees working for companies with more generous benefits may have continuous access, while those with less robust plans may be left without options, despite similar medical needs. This can lead to resentment, decreased morale, and even impact talent attraction and retention for companies perceived as offering inadequate health benefits.
The Broader Healthcare and Economic Landscape
The widespread adoption of GLP-1s and the associated cost concerns are reverberating throughout the broader healthcare ecosystem. Pharmacy Benefit Managers (PBMs), who negotiate drug prices with manufacturers and manage formularies for employers, are at the forefront of this challenge. They are under pressure to secure better discounts, implement step-therapy protocols, and develop innovative pricing models to help employers manage costs. However, the sheer demand and proprietary nature of these drugs limit their leverage to a certain extent.
Pharmaceutical companies, while acknowledging the high cost, argue that the pricing reflects the significant research and development investment, the clinical benefits, and the potential for long-term savings by preventing more expensive obesity-related complications. They also point to patient assistance programs, though these are often limited in scope and duration. The GLP-1 market is a multi-billion dollar segment, driving substantial revenue for pharmaceutical giants like Novo Nordisk and Eli Lilly, who are continuously investing in new formulations and indications.

The impact extends to health insurance premiums across the board. As employers face higher claims for GLP-1s, these costs are factored into renewal rates, contributing to the overall upward trend in healthcare expenditures. This creates a cyclical problem where rising drug costs lead to higher premiums, which in turn place more burden on both employers and employees.
Ethical Considerations and the Balancing Act
The employer’s predicament is not merely financial; it’s also deeply ethical. Companies strive to be good stewards of employee health and well-being, recognizing that a healthy workforce is a productive workforce. Denying or severely restricting access to medications that could dramatically improve an employee’s quality of life and health outcomes can be seen as contrary to this goal. However, unlimited coverage for high-cost drugs, especially for conditions affecting a large segment of the population, could render healthcare benefits unsustainable for the company as a whole.
This necessitates a delicate balancing act. Employers must weigh the immediate financial impact against the potential long-term health benefits, improved productivity, reduced absenteeism, and enhanced employee morale that comprehensive coverage might provide. It also involves navigating the moral imperative to offer effective treatments versus the practical reality of budget constraints. Discussions around medical necessity, the definition of "obesity" as a disease, and the role of employer-sponsored health plans in addressing chronic conditions are becoming increasingly prominent.
Looking Ahead: Future Trends and Policy Implications
The landscape of GLP-1 coverage and cost management is dynamic and will likely continue to evolve rapidly. Several factors will shape its future:
- Newer Generations of GLP-1s and Combination Therapies: Pharmaceutical companies are already developing even more potent drugs, including those that target multiple hormone pathways (e.g., GIP, glucagon receptors alongside GLP-1). While offering potentially greater efficacy, these are also likely to come with even higher price tags.
- Generic Competition: The earliest GLP-1s are still under patent protection, but as patents expire, generic versions could eventually emerge, driving down costs. However, this is still years away for the most popular weight-loss formulations.
- Long-term Outcome Data: More data on the long-term health benefits and cost-effectiveness of GLP-1s will be crucial. If studies conclusively demonstrate significant reductions in cardiovascular events, diabetes complications, and other comorbidities, it could strengthen the argument for broader coverage, as the long-term savings might eventually outweigh the upfront costs.
- Policy Debates: The sheer cost of GLP-1s is prompting national conversations about drug pricing, particularly regarding Medicare coverage for weight-loss medications, which is currently restricted. Any changes at the federal level could have ripple effects on commercial insurance markets and employer strategies.
- Innovative Benefit Designs: Employers, in conjunction with PBMs and consultants, will likely explore more innovative benefit designs. This could include tiered formularies, outcomes-based contracts with pharmaceutical companies (where payments are tied to patient results), or enhanced wellness programs that integrate GLP-1s with intensive lifestyle interventions.
In conclusion, the emergence and widespread adoption of GLP-1 medications represent both a medical triumph and a profound financial challenge for employers. The "tremendous concern" expressed by the Business Group on Health underscores the urgency of this issue. While employers are actively implementing guardrails to manage costs and ensure appropriate use, the underlying high prices and surging demand continue to strain healthcare budgets. Navigating this complex terrain will require ongoing collaboration between employers, PBMs, pharmaceutical companies, and policymakers, all while striving to balance financial sustainability with the ethical imperative to provide access to effective, life-improving treatments for employees. The decisions made today will undoubtedly shape the future of employer-sponsored health benefits and the accessibility of groundbreaking medical innovations for years to come.